| Sabina Fahy, Roy Brown, Darina
Sloan, Shay Keating & John O'Connor
Ir J Psych Med 17(l): 29-33
Objectives: The aim of this study was to examine the prevalence
of, and factors associated with violence in a drug treatment centre.
Method: This study is a retrospective audit of all incident
forms completed at an urban drug treatment centre between December
1991 and July 1996 with reference to case notes for additional clinical
information on individuals involved in violent incidents.
Participants included all patients attending the centre in the aforementioned
time period who were involved in violent incidents. Information
was obtained about the prevalence and severity of violent incidents
and patient details including main drug of abuse, route of use,
reason for attendance, comorbid axis 1 diagnosis, history of previous
incidents and HIV status at the time of the incident.
Results: One per cent of all patients were involved in violent
incidents. Less than one quarter of incidents involved serious injury
or assault. Most perpetrators were male intravenous heroin users
on a methadone maintenance programme. Nurses and doctors were most
frequently the victims of incidents. Ten per cent of patients had
a history of previous incidents and almost half the perpetrators
were HIV positive. A comorbid axis 1 diagnosis was found in 9% of
perpetrators (n = 6), mainly alcohol dependence syndrome.
Conclusions: Those on methadone maintenance programmmes were
most likely to be violent. Almost half the perpetrators involved
in violent incidents were HIV positive. Acute psychiatric problems
did not account for violence in this setting. The presence of on
site security staff probably accounted for the low levels of violence
when compared to general psychiatric settings.
Key words: Violence; Drug Treatment Centre; Drug
abuse.
There is no standardised definition of violence. Fottrell1
described it as, "a generic word bedevilled by the lack of
a universally accepted definition". It can include verbal abuse,
property damage, assault or even life threatening injury.
*Sabina Fahy, Senior Registrar in Psychiatry,
Department of
Psychiatry, University College Hospital, GaIway, Ireland.
Roy Browne, Senior Registrar in Psyclliatry, St Davnet's
Hospital, Monaghan, Ireland.
Darina Sloan, Consultant Psychiatrist, St Ita's Hospital,
Portran:, Co Dublin, Ireland.
Shay Keating, Consultant Psychiatrist, John O'Connor,
Consultant Psychiatrist, Drug Treatment Centre, McCarthy Centre,
30/31 Pearse Street, Dublin 2, Ireland.
*Correspondence
SUBMITTED: JULY 10, 1999. ACCEPTED: FEBRUARY 11, 2000.
Whatever the definition used violence is now a
recognised problem in Accident and Emergency Departments2.3
, psychiatric hospitals and units 4.6 among psychiatric
patients in the community,7.9 and special hospitals.
There is a public perception that drug users are violent which is
supported in the literature.11-13 Previous drug use and
criminal record have been implicated as an associated factor for
violence in a general psychiatric setting.5.14-16 The
aim of this study was to examine all recorded violent incidents
and assess prevalence rates and identify factors associated with
violence in this setting.
The Drug Treatment Centre is an urban based outpatient facility
in Dublin (Ireland) for the specialised assessment and treatment
of persons with substance abuse. It has an average annual attendance
of 47,160 (an attendance is defined as each visit by a patient).
This constitutes an average of 1,500 patients per year. Seventy-six
per cent of those attending are male while 24% are female. The centre
has a staff complement of one consultant psychiatrist and five junior
doctors. Also there is a nursing team (a nursing officer and two
staff nurses), four social workers and three general assistants.
There are two secretarial staff to whom all patients report on their
arrival.
After a full assessment a suitable programme is offered ranging
from supportive counselling, detoxification, maintenance, or harm
reduction. The harm reduction programme consists of patients attending
three nights per week between 6.OOpm-9.OOpm. It aims to encourage
attendance at the centre with standard low dose methadone without
strict urine supervision. This allows access to medical care, needle
exchange and advice on contraception for those whom it is felt would
be unable to comply with a more strict regime. All other patients
attend the clinic daily and give twice weekly supervised urine samples
with additional random testing.
At any given time the proportion of people attending each programme
is as follows:
- maintenance (substitution) programme
70%
- detoxification programme 15%
- harm-reduction (night) programme 15%
These proportions may vary from time to time depending
on clinical needs at the center. All patients must check in at the
secretary's desk so that their chart can be obtained. Patients wait
in a common waiting area which is supervised by security personnel.
In general, patients are seen in individual offices unless it is
felt that there is a potential for confrontation or violence in
which case the interview takes place in the corridor adjacent to
the waiting area out of earshot of other patients but within sight
of the security personnel.
Patients are seen by the doctor at initial assessment and are subsequently
seen for review regarding clinical status which may entail alerting
the patient to a urine sample found positive for various drug groups.
This often results in a reduction or change of
medication. In the event of continued positive urines (despite warnings)
and a decision from the daily team meeting, it is the doctors duty
to inform the patient of a discontinuation of their programme. In
this event they must wait for a further three months before again
applying for a place on the programme.
The patients have daily contact with nursing staff who dispense
medications. In addition the nursing staff may decide that a particular
individual needs to be reviewed by the doctor depending on their
clinical presentation or urine status.
Patients are assessed by social workers for social welfare benefits
and other entitlements and would sometimes represent the patient
as advocates in the setting of a team meeting. They also involve
patients in family therapy and sometimes assist in protection of
children where appropriate. The amount of time that a social worker
spends with each patient varies greatly depending on individual
needs.
All incidents of violence at the Drug Treatment Centre have been
recorded from December 1991. The incident forms record demographic
information and details of the incident and aggressor. All violent
incidents are discussed at the daily team meeting. Depending on
the severity of the current incident and evidence of previous incidents
this results in some patients being placed on a behavioural review
list. This entails being barred from the clinic, which is under
monthly review, by the team. Since 1992 on site security has been
provided by a professional security firm.
Incident forms were examined retrospectively from December 1991
to July 1996. Data was collected about individual incidents regarding
time and location of incident, demographics of perpetrator and person
towards whom violence was directed. Details of the main drug of
abuse, route of use, other prescribed medication, reason for attendance,
comorbid axis I psychiatric diagnosis, history of previous incidents
and HIV status at the time of the incident were obtained from their
medical notes. Violence was graded depending on severity. Grade
1 was defined as verbal abuse or antisocial behaviour, Grade 2 as
property damage and Grade 3 as assault/injury. Data was then coded,
computerised and analysed using SPSS
The perpetrators comprised 46 men and 19 female (the gender of two
patients was not identified). This group had a mean age of 28.4 years
(range 19-42 years). There were 75 incidents committed by 67 patients.
Seven had one previous incident and three had two previous incidents.
Most incidents occurred during weekdays, between 9.OOam and 5.OOpm
(89.3%, n = 72) and in the waiting area (29%, n = 22) or nurses station
(28%, n = 21). Most incidents occurred in 1992 with a decline following
the introduction of on-site security (Fig 1).
At the time of the incident, 97% of perpetrators (n = 73) were using
intravenous heroin. Forty-seven per cent (n = 35) were on a substitution
programme, 24% (n = 18) were on a detoxification programme, 17% (n
= 13) were on a harm reduction program, and 11% (n = 8) had an 'other'
reason for attendance. 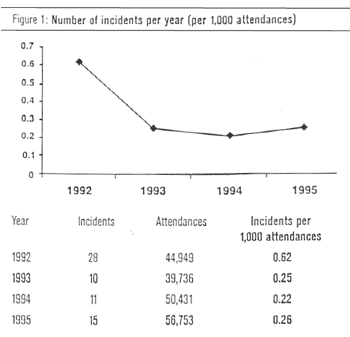
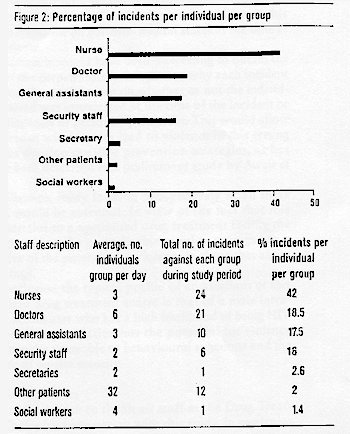
Nurses, doctors and other patients were significantly
more involved in incidents, (X2 = 13.6, df = 6, p = 0.03)
(Fig 2). Six perpetrators had a comorbid axis 1 psychiatric
diagnosis, five of alcohol dependence syndrome and one of schizophrenia.
Eight perpetrators (11%) were on other prescribed medication at
the time of the incident. These included inhalers, antipsychotics
and antiepileptic medication.
The HIV status of 17 perpetrators (23%) was not known at the time
of the incident. Thirty-seven perpetrators (49%) were HIV positive
(whilst the HIV positive rate for the total clinic population was
2%) and 17 were HIV negative (28%). Significantly more males were
HIV positive 30:7 (X2 = 5.3, df = 1, p = 0.02).
Fifty-seven percent (n = 43) of incidents were of type I severity,
20% (n = 15) were type 2 severity and 23% (n = 17) were type 3,
which constituted either an assault or injury. The maintenance group
had more Type 3 incidents (X2 = 7.2, df = 1, p = 0.007).
In 51% (n = 38) incidents perpetrators were placed on a behavioural
review list. In 43% (n = 32) incidents a warning was given and the
outcome was unknown in 5%(n = 5) cases.
The overall rate of violence was 0.03% of all attendances which
constitutes 1% of patients who attended the clinic annually. This
rate was much lower than rates reported in general psychiatric settings
as was our rate of recidivism at 10%.5.10.17 In addition
less than a quarter of all incidents resulted in serious injury
or assault. These findings may be attributable to: a) the introduction
of security staff in 1992 acting as a possible deterrent (Fig
1), b) behaviour modification programmes in existence at the
centre resulting in sanctions depending on behaviour, c) under-reporting
of incidents due to the retrospective nature of the study.18
The study demonstrated increased prevalence of male perpetrators
which reflects the male/female distribution that exists at the clinic
generally. D'Orban19 cites a male: female ratio of 9:1
for violence against the person in the UK. A study by Larkin10
referring to a special hospital found an increased rate of violence
in women patients.
The decrease in incidents at weekends concurs
with previous studies and probably reflects fewer changes in clinical
management or medication.5
Doctors were involved in almost as many incidents as nurses (Fig
2). However, there are twice as many medical staff at the centre
than nursing staff so the comparative risk to nurses is greater.
Other studies of violence also show nurses in the majority.5.16
The increased risk of violence towards nurses and doctors probably
reflects the type of interaction they have with the drug abuser.
As expected, nurses were involved in almost a quarter of all incidents,
indicative of the amount of total contact with the patient in initial
contact and dispensing of medications.
The doctors' role involves informing the patient of discontinuation
of their programme and warnings regarding positive urines which
can be potentially confrontational particularly in an intoxicated
individual. Interestingly social workers were involved in very few
incidents despite regular and frequent contact with some individuals.
Social workers were probably perceived by the drug abuser in a more
supportive and less potentially confrontational role than either
nurses or doctors.
Intravenous heroin was the most common primary drug of misuse reflecting
the drug using patterns of the general population at that time (Drug
Treatment Centre Board Statistics for 1992-1995). The majority of
perpetrators (48%) were on a methadone maintenance programme reflecting
the overall proportions attending the clinic (ie.70% of all clinic
patients are on a substitution programme). interestingly, a higher
proportion of detoxification patients (24%) were involved in incidents
(as opposed to15% of the general clinic population). This may be
related to their difficulty in coping with opiate detoxification.
Almost half the perpetrators were HIV positive
which is much higher than the rate of 2% for the overall clinic
population. This finding may indicate antisocial personality traits
or chronicity of drug use among the violent group. A diagnosis of
antisocial personality disorder has previously been found to increase
the risk of sharing injection equipment with increased rates of
HIV.20. Organic factors might also be contributory. In
addition these HIV positive patients may reflect a sub-group who
have a higher risk taking potential in general and thus perceive
that they have little to lose by being confrontational. Further
prospective study of these hypotheses may elucidate possible cause
and effect factors as to the high proportion of HIV positive perpetrators
of violence.
Only 9% of patients were found to have a comorbid axis I psychiatric
diagnosis and all but one of these patients suffered from alcohol
dependence syndrome. This suggests that acute psychiatric symptoms
did not account for the violence seen in this setting of a specialised
drug treatment centre but the co-abuse of alcohol does contribute
to the potential for violence in this population.
As a result of these findings a contract has recently been introduced.
This lists behaviours that are deemed to be unacceptable and outlines
the consequences of same. Each client is required to sign the contract
before the initiation of their treatment programme and this is kept
in their chart for reference in the event of any changes in their
management.
Some limitations of this study include the fact that it is retrospective
and as such our information obtained from the incident forms and
chart reviews may be incomplete. By necessity out information is
limited to the accuracy of historical clinical notes which limits
the ability of this study to comment on patients' mental states
at the time of the incidents.
In addition it would have been interesting to obtain the views of
the perpetrators in relation to why each incident arose and also
to comment on whether or not the individual involved was intoxicated
at the time of the incident or had a diagnosis of personality disorder.
This would allow us to predict what factors lead to violence in
this setting and thus develop possible prevention strategies, as
has already been described in a preliminary study by AwaIt et al21
A follow-on study looking prospectively at all these factors would
be essential. In view of the fact that this study pertains to a
specialised drug treatment facility the findings may not be generalisable
to other settings but is indicative of the potential for violence
in those that abuse illicit drugs.
In conclusion the typical profile of an assailant at this specialised
drug treatment centre is that of a male intravenous heroin user
who has a high likelihood of being HIV positive. This population
has the potential for violence which may be amenable to behavioural
sanctions and the presence of on-site security.
The authors wish to thank all staff at the Drug Treatment Centre
for cooperation with this study, in particular the secretarial and
nursing staff.
1. Fottrell E. A study of violent behaviour
among patients in psychriatric hosptials. BL Psych 1980: 136:216-21
2. Wyatt JP, Watt M. Violence towards junior doctors in accidnet
and emergency departments, J Acc Emerg Med 1995: 12: 40-2
3. Cembrowicz SP, Shepard JP. Violence in the
accidnet and emergency department. Med Sci Law 1992: 32(2): 118-22
4. Schwartz TL, Park TL. Assaults be patients
on psychiatric residents: a survey and training recommendations.
Psychiatr Serv 1999: 50(3): 381-3
5. Walker Z, Seifert R. Violent incidents in a
psychiatric intensive care unit. B J Psych 1994: 164: 826-8
6. Aquilina C. Violence by psychiatric in patients.
Med Sci Law 1991:31(4):306-12
7. Streadman HJ. Mulvey EP. Monahan J et al. Violence
by people discharged from acute psychiatric inpatient facilities
and by others in the same neighbourhoods. Arch Gen Psychiatry 1998:
55: 393-401
8. Scott H. Johnson S. Menezes P et al. substance misuse and the
risk of aggression and offending among the severly mentally ill.
B J Psychiatry 1998: 172: 345-50
9. Swanson J. Borum R. Swarrz M Hiday V. Violent
behavior preceding hospitalisation among persons with severe mental
illisess. Law Hum Behav 1999; 23(2): 185-204.
10. Larkin E. Murtagh S, Jones S. A preliminary study of violent
incidents in a special hospital (Rampton). B J Psych 1988; 153:226-31.
11. Ball JC. Rosen L. Flueck JA. & Nurco DN.
Lifetime criminality of heroin addicts in the United States. J Drug
Issues, 1982: 12:225-9.
12. Kouri EM. Pope HG. Powell KF. Oliva PS. Campbell
C. Drug use history and crimial behavior among 133 incarcerated
men. Am J Drug Alcohol Abuse 1997:23(3): 413-9.
13. Hanlon TE, Nuren DN, Kinlock TM, Duszynski
KR, Trends in criminal activity and drug use over an addiciton career.
Am J Drug alcohol Abuse 1990:16: 223-38
14. Tardiff K, Marzuk PM, Leon AC, Portera L,
Weiner C. Violence by patients admitted to a private psychiatric
hospital. Am J Psychiatry 1997:154(1):88-93
15. Cuffel BJ, shunway M, chouljian TL, MacDonald
T. A longitudinal study of substance use and community violence
in schizophrenia. J Nerv Ment Dis 1994:182:704-8
16. Swartz MS, Swanson JW, Hiday VA, Borum R,
Wagner HR, Burns BJ. Violence and severe mental illness: the effects
of substance abuse and nonadherence to medication. Am J psych 1998:
155(2): 226-31
17. James DV, Fineberg NA, Shah AK, Priest RG.
An increase of violence on an acute psychiatric ward: a study of
associated factors. B J Psych 1990: 156:846-52
18. Haller RM, Deluty RH. assaults on staff by
psychiatric in-patients - a critical review. B J Psych 1988:152:174-9
19 D'Orban P. Female Offenders. In: Gunn J, Taylor P (eds). Forensic
Psychiatry - Clinical. Legal and Ethical Issues. Butterworth Heinemann
1993:600.
20. Brooner RK, Bigelow GE, Strain E, Schmidr
CW. Intravenous drug abusers with anti-social personality disorder:
increased HIV risk behavior. Drug AlcoholDepend 1990:26(1): 39-44
21. Awalt RM, Reilly PM, Shopshire MS. The angry
patient: an intervention fro managing anger in substance abuse treatment.
J Psychoactive Drugs 1997: 29(4): 353-8
|

